Radiology of low back pain
After taking a thorough history, and performing a detailed physical
examination, radiological confirmation is important. After all, this
is a picture which tells the physician whether or not there is something
mechanically present which may explain the symptoms.
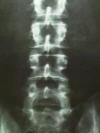 An
AP (anterior to posterior ) film of the lumbar spine is looking through the
body, from front to back. This type of view can spot fractures,
and is often useful for early detection of tumors involving the bone. An
AP (anterior to posterior ) film of the lumbar spine is looking through the
body, from front to back. This type of view can spot fractures,
and is often useful for early detection of tumors involving the bone.
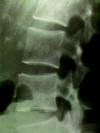
A lateral x ray of the lumbar spine is excellent for
determining alignment of the spine. Compression fractures can detected
easily. In addition, collapse of the disk spaces may indicate
degenerative disk disease.
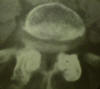
A CT (computed axial tomography) scan shows "slices"
through the lumbar spine. This type of image uses x rays, delivered in
a circular manner circumferentially around the body. A sophisticated
computer then adds the various rays, calculates densities of bones and soft
tissue within the center of the rays, and produces a picture. The
first CT scanner was made by EMI (which also produced Beatles records), and
was extremely slow, and the pictures were relatively poor, by today's
standards. Present day CT scans are fast, and quite sharp. CT is
best for looking at bone, while soft tissue within the lumbar spine (such as
nerves and herniated disks) are less optimally seen.
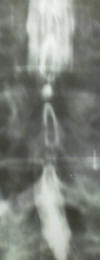
A myelogram is a study in which a spinal tap is performed
within the lumbar spine, and radioopaque (shows up on x-ray) dye is placed
within the spinal fluid. X-rays are then taken, and CT scans are taken
as well. The dye provides an outline of the nerves, and any
abnormality, such as a herniated disk, can be seen as an indentation or
defect in the normal filling of dye. In the myelogram on the left, the
normal column of white dye is significantly narrowed by compression upon the
nerves.
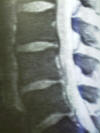
MRI (magnetic resonance imaging) provides exquisite views
of the nerves and other soft tissues around the lumber spine. While
they don't provide as much detail about the bone as a CT scan does, they do
offer the advantage of showing images in many different planes (axial,
coronal, sagittal). Sometimes herniated disks which are subtle and
difficult to see in one plane, are easily seen in another. These scans
rely on magnetization of hydrogen atoms, and so far have not been found to
have any long lasting adverse risks. Some patients have difficulty
because the "bore" into which they must lie is relatively narrow, and "open"
MRI scanners suit these patients better. Unfortunately there is some
compromise of image quality in the open MRI scanners, and the closed
machines of comparable technology still provide the best pictures.
A discogram is a study in which radioopaque dye is
injected into the disk space. This is both an anatomical study as well
as a functional study. It looks at the anatomy of the disk space, and
can show when dye leaks through rents in the annulus fibrosis. But
just as or even more important, it is a functional test. When the
physician injects dye into the disk space, the patient reports, on a scale
from 1 to 10, how much pain has been produced. If the pressure
injection of dye into the disk space reproduces the patients usual low back
pain, then surgical fusion of the disk space may have some benefit in
improving the pain. As far as the low back team knows, it is the only
test in which we hope a patient has significant pain, because that means the
disk is likely a cause of the pain, and surgical fusion may help. This
is usually a method of last resort, after all else has failed. |

